NHS staff defended by retired surgeon over vaccinations
We use your sign-up to provide content in ways you’ve consented to and to improve our understanding of you. This may include adverts from us and 3rd parties based on our understanding. You can unsubscribe at any time. More info
Camcon Medical say their oxygen delivery platform, which uses devices known as iMOD and BiMOD, could free up NHS bed space and ease pressure on nurses who have been under tremendous strain during the pandemic. The technology works by delivering a pulse of oxygen which travels to the parts of the lung not damaged by the killer virus. Camcon Medical claim this is the first new medicinal gas delivery device for oxygen in 100 years.
Specifically, BiMOD delivers oxygen along with nitric oxide to allow enhanced blood flow and greater oxygen uptake in the lungs.
Danny Chapchal, Chairman, Camcon Medical, explained: “It uses advanced engineering to deliver precise amounts of medicinal gases, such as oxygen, at the optimal time in each inhalation to allow added oxygen to reach the best areas of the lung for oxygen uptake.”
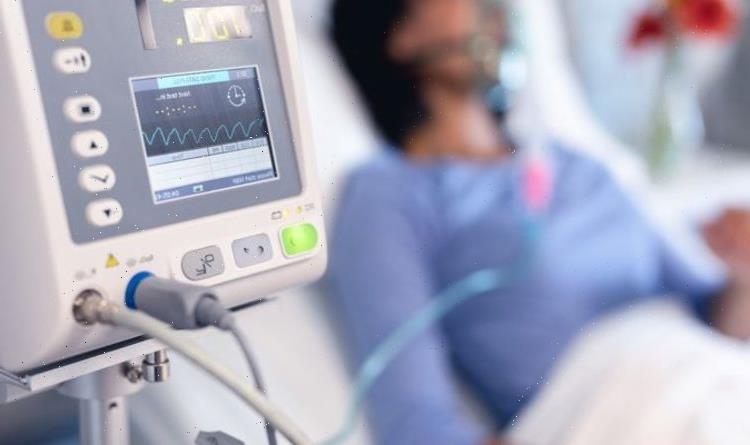
But instead of being unconscious, the patient wears a mask or nasal cannula linked to the device. They can still talk, drink and eat.
Mr Chapcal added: “Its aim as a fully automated delivery system is to reduce the work of clinicians in Intensive Care Units (ICUs) and, in future, enable patients to use the device at home.”
Experts from Camcon Medical told Express.co.uk that there is scope for the technology to save lives.


They explained: “It is designed to avoid putting patients on Invasive Mechanical Ventilation (IMV) which is traditionally used for severe respiratory failure.
“The mortality rate of IMV is 40 percent.
“As a guide, in January 2021 there were 4,076 Covid patients in ventilator beds on one day.
“From April 2019 to March 2020 there were 146,371 patients admitted into acute Intensive care units (ICUs) in the 194 units in England and Wales.
“Some 33 percent – or 48,300 – of these received invasive mechanical ventilation (IMV).

“40 percent of that is 19,300 patients who were in ICU on ventilators who, according to the mortality rates – would have died.”
And Camcon Medical seemed certain that it will allow NHS bed space to free up.
They told Express.co.uk: “The main reason hospitals get so busy during winter is the increased demand for bed space and clinical staff to care for those patients on wards.
“A ventilated patient requires intensive monitoring and treatment – it could take 7 people to turn them over for example.
“But mechanical ventilation is also not a quick fix – it’s a long process with patients spending an average of 8 days on IMV.”
DON’T MISS
NASA offering $1m to come up with ‘innovative’ solution to dilemma [REPORT]
UK scrambles to bolsters gas supplies as Russia threatens blackouts [REVEAL]
Millions of Britons face blackouts as emergency supplies triggered [INSIGHT]


They also believe that the technology could completely change the way respiratory illnesses are treated.
They told Express.co.uk: “It is not just about freeing up ventilator beds, it is about replacing that 100-year-old method of treating respiratory failure with 21st-century technology for patients who could still breathe if their lungs get oxygen into the right places.
“If you also have a treatment where patients who are in hospital because they need help with breathing can be in chairs, eating and speaking or can even go home and use the equipment, then you have increased bed space and decreased the workload for NHS staff who can then be deployed elsewhere.”
Source: Read Full Article