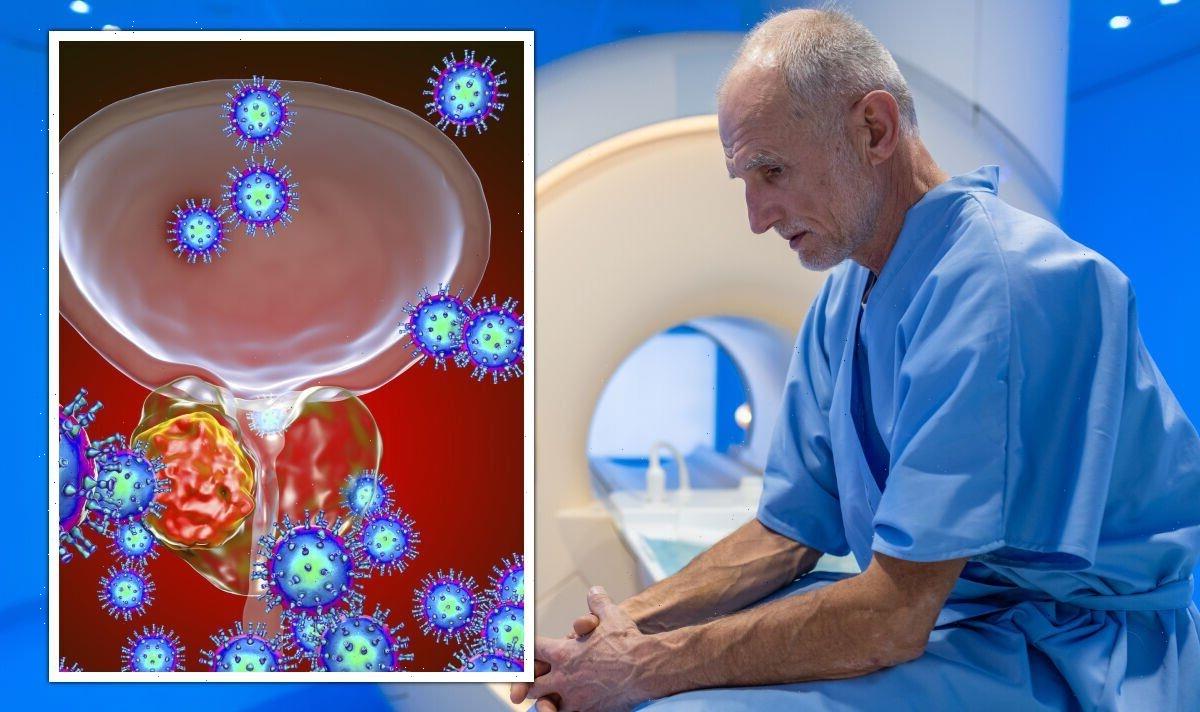
Prostate cancer: Doctor outlines symptoms you might experience
We use your sign-up to provide content in ways you’ve consented to and to improve our understanding of you. This may include adverts from us and 3rd parties based on our understanding. You can unsubscribe at any time. More info
A third of patients in Scotland were diagnosed after their cancer had spread beyond the gland, compared with one in eight in London, a charity warned. But there was also significant variation within England. One in five cases were caught late in the worst-performing region – the North East and Yorkshire – according to Prostate Cancer UK.
The charity’s chief executive, Laura Kerby, said: “Every man should get an equal chance of a cure.
“This postcode lottery for cancer diagnosis simply isn’t fair and the picture in Scotland is particularly shocking.
“Unfortunately, early prostate cancer usually doesn’t have any symptoms, which is why men need to be aware of their risk and should take our online risk checker to find out more.
“If you’re at higher risk – which includes all men over 50 – you’re entitled to a free PSA blood test from your GP.”

Nearly 10,000 men every year are diagnosed with stage four incurable prostate cancer – after the disease has spread around the body – in the UK.
Men who are at high risk can undergo a PSA test, which measures the amount of prostate specific antigen in the blood.
If the level is above normal, the patient may be sent for further checks with a specialist.
The charity is urging GPs to discuss the benefits of the PSA test with high-risk patients, so they can make an informed choice about whether to have it.
Separate data has also shown shows men living in more deprived areas are more likely to be diagnosed late.
There was a worrying 29 per cent drop in diagnoses during the first year of the Covid outbreak, meaning yet more cases may be found at the incurable stage.
Prostate Cancer UK said the backlog was beginning to clear in England, with referrals now above pre-Covid levels.
However, the speed of recovery varies between regions.
In October last year, referrals in London were at 19 per cent above pre-pandemic levels, but only up five per cent in the Midlands.
Ms Kerby said: “At one point in the pandemic, prostate cancer made up a third of all missing cancer cases.
“So it’s fantastic to see that we are beginning to locate and treat all these men. However, there is still a long way to go to fully reverse the impact of the pandemic. And as these figures show, our job isn’t done even then.
“That’s why we need a screening programme for prostate cancer, and we are committed to funding the research to make this a
reality and save thousands of men’s lives.”
- You can identify your risk by using Prostate Cancer UK’s online checker, at prostatecanceruk.org/riskcheck
‘Get checked…this doesn’t have to happen to others’
Surgeon Gareth Jones is urging other men to be aware of their health after he was diagnosed with advanced prostate cancer.
His disease was spotted only after it had spread to his bones in June 2021.
Gareth, 55, from Glasgow, had always been generally fit and healthy, before he started to notice “niggling injuries”, such as back pain.
He said: “Little did I know this was a sign my cancer had already spread to my bones.
“Being diagnosed was very, very difficult, but thankfully I started my treatment that same day so there were no delays.”
He added: “I’m determined to live life to the full and I’m now back in the gym and am doing what I can to raise awareness.”
Gareth has raised more than £4,000 for Prostate Cancer UK through sponsored fitness events including a 180-mile swimming and walking challenge in Switzerland.
He said: “I just don’t want this to happen to other men. It can be avoided if more men know about prostate cancer and what to do about it. That’s why I would tell anyone and everyone to share Prostate Cancer UK’s risk checker.
“We need to get the message out there and stop so many men missing out on an early diagnosis.”
Source: Read Full Article