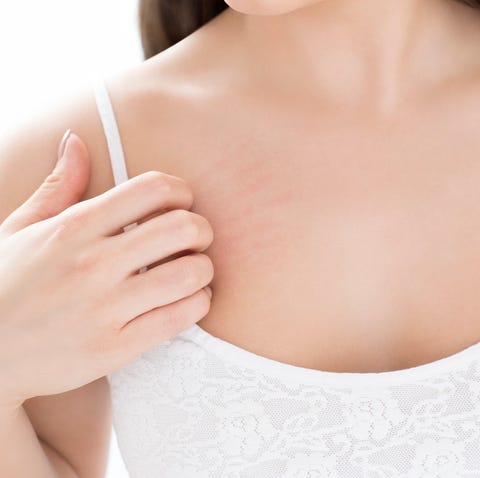
Of all the inconvenient places to have itchy skin, your breasts and nipples rank pretty high. I mean, you can’t just rub calamine lotion all over your boobs, right (nor would you want to, TBH).
There’s a bunch of reasons why you might be spending too much time feeling yourself up in public—and most of them are pretty harmless. Still, it helps to know what exactly is causing that super-annoying itching, so you can know how to treat it.
If itching is actually driving you crazy, it’s best to book an appointment with your ob-gyn—in the meantime, here are 12 reasons why you just can’t stop scratching your boobs, and what you can do about it.
1. You have eczema.
Eczema is a genetic skin disorder often made worse by environmental exposures, says Kari Martin, M.D., assistant professor of dermatology at the University of Missouri School of Medicine.

An eczema rash has a pretty specific look: it’s often categorized as small raised bumps or reddish patches on the skin, and it can definitely show up on your nipples—but Martin says the rash will likely appear on both your nipples and breasts.
You can try to treat eczema on your own—Martin recommends avoiding harsh soaps and moisturizing the skin regularly with an emollient such as petroleum jelly. You can also try an OTC hydrocortisone ointment twice a day for up to two weeks, but check with your dermatologist if it doesn’t clear up after that.
2. You have psoriasis
Like eczema, psoriasis is another skin condition—but this one is caused by an autoimmune disorder.

Psoriasis also has a tell-tale look: red, scaly plaques on the skin, most commonly on the outsides of your elbows and knees, says Martin. But the rash can appear anywhere–including your breasts and nipples. You’ll want to see a dermatologist for this one too, but in the meantime, Martin recommends trying hydrocortisone ointment for any psoriasis-related itching.
3. You’re currently using narcotics.
There are a lot of reasons why your doctor might prescribe an opioid pain reliever—severe migraines, broken bones, surgery—but while the narcotic is working to ease your pain, it might also be causing you to itch.
If your bras don’t fit (or you go braless a lot), you might end up with itching and chafing.
“Some narcotics have been reported to cause a release of histamine from cells in the body, which can cause generalized pruritus [itchy skin],” says Stephanie Gore, M.D., an ob-gyn at CareMount Medical.
To combat the itch, take an oatmeal bath and keep your skin well-moisturized; if your doctor approves it, you can also try taking an antihistamine, says Gore. Switching to a different medication, when possible, may also help.
4. You have an insect bite.
Insect bites might not be the first thing you think of when you’ve got an annoying itch on your breast, but it’s totally possible. Gore says to inspect the area carefully for signs of an insect bite—like a single raised bump and redness surrounding it—and pay special attention to marks that appear in multiples, since that could mean you have a bed bug infestation (gross, but true).
OTC hydrocortisone creams, calamine lotion, or oral antihistamines are usually a good defense against itchiness from insect bites, says Gore.
5. You’ve had radiation therapy for breast cancer.
Radiation therapy for breast cancer can lead to a specific type of dermatitis (a.k.a., inflammation of the skin), and Martin says the itching can start right after the patch of skin has been exposed to radiation, or even months or years later.

“It occurs because of damage and scarring [from] the radiation beams passing through the skin to deeper tissues,” she says. “It usually presents as broken blood vessels and firmness of the skin; it may be painful, itchy, or have no associated symptoms at all.”
Like with most forms of dermatitis, moisturization is key—but sometimes stronger topical corticosteroids are needed, in which case Martin recommends heading to your ob-gyn.
6. You’re pregnant.
If you’re expecting, you can also expect some itching to go along with that growing baby bump. Gore says normal physiological changes that occur during pregnancy, like the enlargement of the breast in preparation for lactation, can be enough to cause a woman’s breast to itch.
“As the skin stretches to accommodate the [growing] breast, it often becomes dry and irritated,” she explains. “Some women develop stretch marks, which irritates the skin even more.” The best way to manage symptoms? Keep the skin moisturized with topical lotions—specifically unscented ones, to avoid further irritation, says Gore.
7. You’re breastfeeding.
Intensive breastfeeding (like during the newborn period) can cause itch-inducing dryness, says Gore. Your ob-gyn can recommend a few baby-safe remedies—like medical grade lanolin or even warm compresses—to try if your nipples have become seriously dry or cracked from breastfeeding.
A rare form of cancer called Paget’s disease can cause itching on the breast.
But this broken skin can also lead to the introduction of bacteria into the milk ducts, which may result in an infection called mastitis, says Gore. Mastitis, which can also be caused by an overgrowth of bacteria in the breast milk thanks to infrequent feedings or blocked milk ducts, causes symptoms like pain or tenderness in the breast, as well as fever and flu-like symptoms. If you think you have mastitis, call your doctor, since you may need an antibiotic.
8. You’re allergic to that new lotion you’re using.
This is called allergic contact dermatitis, which “occurs when someone becomes allergic to a chemical [that comes] in contact with their skin,” says Martin. “[On] the nipples, this would most often be metal in a piercing, an OTC medication or skin-care product being used on that skin, or more rarely, preservatives in clothing.”

This kind of dermatitis leads to a pink or red rash that’s dry and itchy. Martin says it may be localized or more widespread, and could even lead to blistering and crusting. OTC hydrocortisone might help, but keep an eye on it—you’ll need to make an appointment with your doctor if it doesn’t improve.
9. Your breast is rubbing against your bra a little too much.
Irritant contact dermatitis also leads to pink and scaly or dry plaques, says Martin, and can be caused by excessive dryness from harsh cleansers or friction—on the breasts and nipples in particular. So if your bras are ill-fitting (or you frequently don’t wear one at all), you might end up with chafing and irritation.

Friction can also happen if your breasts are asymmetrical, i.e. one breast is a larger cup size than the other, leaving the smaller one to move around more in the cup. Get yourself a proper bra fitting from a professional, and consider investing in bras designed to accommodate uneven or differently sized breasts.
10. You’ve recently had breast surgery.
If you’ve recently had any kind of breast surgery, you’re probably expecting pain, soreness, or tenderness in the days after—as well as (unfortunately) itching.
“After surgery, as part of the healing process, histamine is released and swelling of the breast occurs,” says Lyda E. Rojas Carroll, M.D., a general surgeon who specializes in breast surgery at CareMount Medical. “That may stimulate nerve endings and cause itching.” To alleviate the itching caused by swelling, Carroll recommends wearing a surgical bra and applying ice.
11. You have a rare type of breast cancer.
It’s an unlikely cause of your itching, but technically Paget’s disease of the breast is a possibility. This rare type of breast cancer occurs in the nipple then spreads to the areola, and shows up as a red, scaly rash that doesn’t get better after use of topical creams, says Carroll.
“The itching is caused by the local skin reacting to the cancer cells growing within the nipple,” Carroll explains, adding that it’s extremely rare to have Paget’s in both nipples (so if your itching or rash isn’t exclusive to one side, it’s even less likely you have it). Still, if you’re concerned, make an appointment with your doctor; surgical treatment would likely be recommended.
While we’re at it, make sure to get regular dermatology cancer screenings, too—Carroll says skin cancer of the breast (basal cell, squamous cell, and melanoma) can also cause itching.
12. You have a yeast or fungal infection.
Chances are, you’ve had a vaginal yeast infection before, but the infection can show up on your boobs too.
There are a few different kinds of yeast infections you might find on your breasts, ranging from nipple and areola infections common with breastfeeding to infections in the fold of the skin under the breasts (thanks to the sweat and moisture that gets trapped there), says Martin. These itchy rashes vary in color—either pinkish red, yellow-orange, or pinkish white—and are usually circular patches that may have a fine scale over the top.
“Topical antifungal medications such as clotrimazole or miconazole creams twice daily can be helpful in many cases,” explains Martin. “For rashes under the breasts, keeping the skin as dry as possible and keeping a layer of clothing (like a well-fitted bra or handkerchief) between skin folds is also helpful.”
Source: Read Full Article